What Happens Right Before and After Giving Birth?
For most mothers-to-be, childbirth is the finish line after a nine-month journey. The big day ideally arrives between 37 and 42 weeks of pregnancy. No matter how excited and ready pregnant mothers are, childbirth is both miraculous and frightening. Today, mothers have many options when it comes to how they want to give birth. Keeping an open mind and focusing on the arrival of your new baby can remove some of the trepidation from the birth experience.
Three Stages of Childbirth
Every delivery is unique, but most labors and deliveries follow the same pattern. The first stage includes two phases: early and active. During early labor, the cervix thins out, then dilates or opens so that the baby can pass through. Then, active labor begins; the contractions intensify as the baby moves into the birth canal. In the second stage, which starts at about 3 to 4 cm dilation, the woman reaches full dilation of 10 centimeters, and she can begin pushing or bearing down. The baby is born during the third stage, and, finally, the mother expels the afterbirth, placenta, and membranes.

Vaginal vs Cesarean Birth Delivery
A vaginal delivery is one that requires very little or no medical intervention. A doctor may perform an assisted vaginal delivery using forceps or a vacuum device, but these interventions make up only about 3% of births. In some cases, issues require the medical staff to abruptly switch tactics to a Cesarean delivery or C-section if the doctor determines that vaginal delivery is not safe for the mother or child. The physician makes a vertical or transverse incision through the mother's abdomen and uterus to open the amniotic sac and deliver the baby. In most cases, the mother remains awake during the procedure. In some situations, pre-existing medical conditions or issues related to the baby or mother's health may result in the scheduling of a C-section for just before a woman is expected to go into labor.

Emergency Cesarean Delivery
Sometimes, there are no indications that a C-section is necessary until after labor has begun. If the baby's heart rate is abnormal, below 120 beats per minute or above 160 beats, and other medical intervention does not remedy the issue, the physician may decide to do a C-section. If the labor does not progress normally in other ways, such as if the baby is in a position that makes delivery difficult or impossible, this may also result in an unplanned C-section.

Labor Induction
If a woman does not go into labor within two weeks beyond her due date, a physician could choose to induce labor. Statistics show that approximately one out of every four women have their labor induced. The doctor will stimulate the uterine contractions that instigate labor. Women who have had a previous C-section or breech or sideways baby placement in the uterus may not have the option for labor induction. It is also not an option for women with placenta previa, where the placenta is blocking the cervix. Most obstetricians discourage labor induction for convenience reasons and recommend that it only be used if there is a medical need.

Hormones Assist With Delivery
A mother's body produces hormones that not only trigger labor but also help during and after childbirth. A hormone called prostaglandin helps the cervix open. Relaxin softens and stretches the cervix to prepare for birth. Oxytocin causes contractions during labor, then helps the body deliver the placenta after the baby is born. It also helps the uterus shrink back to its normal size following the birth process, and it works with another hormone called prolactin to spur breast milk production. A surge of beta-endorphins, the pleasure hormones, help reduce pain. Extreme stress during labor can lead to excessive beta-endorphins, however, which can inhibit oxytocin release and slow down the labor process.

Home Births, Birthing Centers, and Hospitals
Expectant mothers have choices when it comes to the birth experience. Some women wish to give birth without medical intervention, in a familiar place. While home births may be an acceptable alternative for some women, physicians generally advise against them for those who are pregnant with multiples, have a baby who is not in a headfirst position, or have had a previous C-section. They also advise that women who choose home births have a certified nurse-midwife or trained health care provider such as a doula to assist them. Some mothers choose certified birthing centers or hospitals, which the medical community considers the best and safest option, in case complications arise during labor or delivery.

Water Immersion Deliveries
Although the American College of Obstetricians and Gynecologists (ACOG) do not recommend it, water immersion has become a popular birthing method in recent decades. Proponents claim this alternative method not only decreases pain during the first stage of labor, but decreases labor duration. One study shows that women who have had a C-section may have a better chance of a vaginal birth with a water immersion delivery. The study also indicates no difference between those infants born through immersion births and those born on land. However, there have been rare occurrences of adverse effects in newborns following immersion births, according to the American Academy of Pediatrics.

Episiotomy
Once a routine part of childbirth, many physicians no longer recommend episiotomies, incisions in the perineum tissue area between the anus and the vaginal opening. Sometimes, the perineal area tears during the birth process. Obstetricians once believed that episiotomies were necessary to make a larger vaginal opening and prevent tearing. In 2006, however, the ACOG recommended that physicians restrict the use of episiotomies because the procedure does not benefit either the mother or infant. Doctors may still take this step in the case of severe maternal lacerations and difficult deliveries.

Delivery Medications
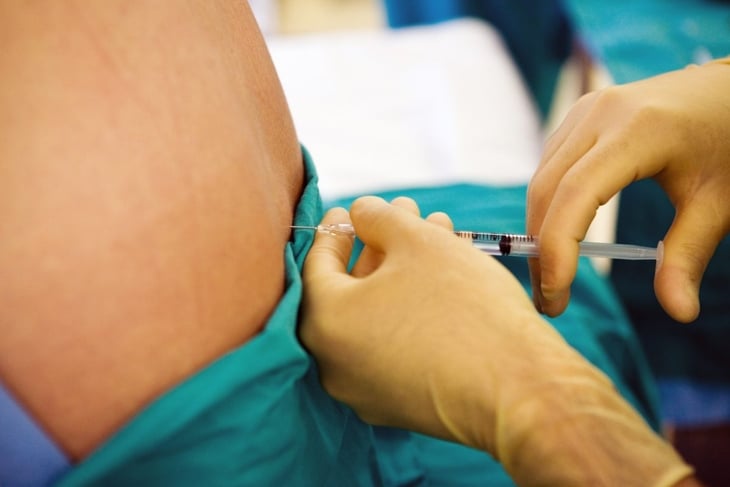
Leading up to the delivery, a variety of medications can ease pain. [citation href='https://www.mayoclinic.org/healthy-lifestyle/labor-and-delivery/in-depth/labor-and-delivery/art-20049326" title="Mayo Clinic" desc="Labor and delivery: Pain medications"]Epidurals and spinal blocks are the most common choices, but there are other options. Determining the best medication for the delivery beforehand is crucial for a healthy and safe birth. Both epidurals and spinal blocks alleviate most of the pain, usually without affecting labor. However, if the technician makes a mistake, these medications can lower blood pressure and affect the child. Other options include opioids, local anesthetics, and nitrous oxide, though these are not ideal for most deliveries.
Following Delivery
After delivery, the physician or birth attendant will clamp the umbilical cord, cut it close to the infant's navel, then conduct a set of tests called the Apgars. These tests measure the newborn's breathing, muscle tone, color, reflex response, and heart rate to assess overall health. If the mother had an episiotomy or there was severe tearing, the physician will suture the perineum and also check for vaginal blood loss. Additionally, a member of the birthing team will examine the firmness of the top of the uterus to check for hemorrhage. If the physician performed a C-section, they will close the incision. An attendant then places the baby onto the mother's chest for skin-to-skin contact.

Scroll Down
for the Next Article
Popular Now on Facty Health
Disclaimer
This site offers information designed for educational purposes only. You should not rely on any information on this site as a substitute for professional medical advice, diagnosis, treatment, or as a substitute for, professional counseling care, advice, diagnosis, or treatment. If you have any concerns or questions about your health, you should always consult with a physician or other healthcare professional.