It is scary when a simple stomach ache or muscle cramp becomes a trip to the emergency room. Hemoperitoneum, a form of internal bleeding that flows into the peritoneal cavity or abdominal cavity, can cause this event. A person should seek immediate medical care if what they assumed was a stomach ache begins to worsen.
Dialysis
Both peritoneal dialysis and hemodialysis have their risks of accumulated blood in the belly. In the case of peritoneal dialysis, the lining of the peritoneum filters the blood, while a cleaning solution runs through the body. One study showed that some women of reproductive age who were receiving peritoneal dialysis developed recurrent mid-cycle episodes of hemoperitoneum. The causes ranged from ovulation to ruptured luteal or ovarian cysts. Another case demonstrated that the arteriovenous fistula (AVF) created by doctors to facilitate hemodialysis can weaken the vein wall, increasing the risk of an AVF aneurysm.

Solid Organ Blunt Trauma
A collision, such as a car accident, can cause blunt force trauma to the abdominal and pelvic regions, especially in the rectouterine pouch between the uterus and the rectum. Trauma to any of the organs in this area, which is home to the liver and spleen, can cause bleeding into the peritoneal cavity. Small amounts of blood in the rectouterine pouch is a key indicator of intraperitoneal bleeding and will prompt doctors to find the source.

Aortic Aneurysm
An aneurysm is a balloon-like bulge in a section of the aortic artery, which extends from the heart all the way down to the abdomen and branches out into the lower limbs. Aortic aneurysms, specifically, are responsible for nearly 10,000 deaths in the U.S. The major reason for these deaths is their tendency to suddenly rupture and bleed into the cavity. Unfortunately, unless diagnosed and treated quickly, aortic aneurysms become life-threatening.

Extrauterine Pregnancy
Extrauterine pregnancies — when the fertilized egg implants outside the uterus — are life-threatening conditions that have close to a 20% mortality rate. Two examples are ectopic pregnancy, which happens in the fallopian tubes, and tubal rupture, which can cause implantation in the peritoneum. When this happens, it takes between five and seven weeks for peritoneal bleeding and acute abdominal pain to occur.

Nausea and Vomiting
Part of the peritoneum has nerves feeding it at the submesothelial level. This region is extremely sensitive to noxious stimuli, which can cause friction and inflammation. Hemoperitoneum causes inflammation in the surrounding tissues and organs, including the gastrointestinal tract, which results in neurons triggering nausea and vomiting.

Kehr’s Sign
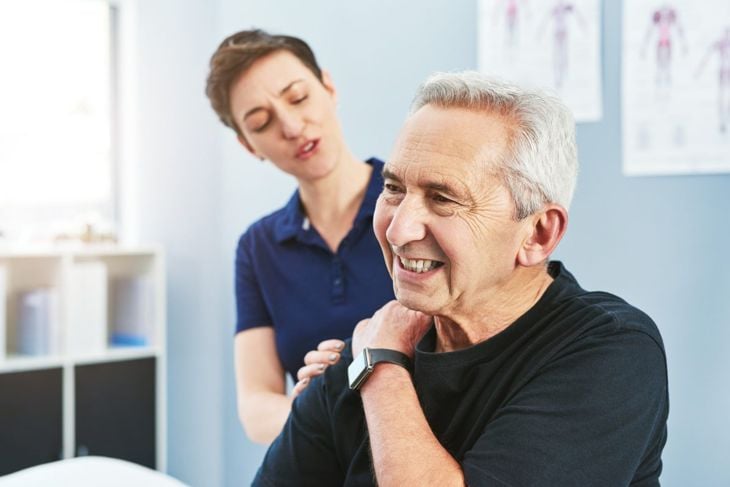
Hemoperitoneum causes pain and tenderness in the abdominal and pelvic regions, but another, unexpected symptom is shoulder pain. Kehr’s sign is acute shoulder pain referred by the phrenic nerve, which extends to the diaphragm. The sensation is triggered by a foreign substance in the peritoneum. Kehr’s sign is considered a classic symptom of a splenic injury that has become a bleeding laceration.
Hypovolemic Shock
During hemoperitoneum, the decrease in blood volume can be sudden and significant. As the cavity can hold much of the body's blood during dialysis, hypovolemic shock is a possibility following trauma such as an aortic aneurysm. This level of blood loss robs the brain of its vital supply, causing dizziness and confusion, which can lead to unconsciousness. The sudden pooling of blood can also leave the skin cold and clammy.

Delayed Hemoperitoneum
Delayed hemoperitoneum is a rare complication. In this case, symptoms may take days or weeks to manifest. Initial signs include generalized abdominal pain that is easily mistaken for another ailment. At some point, however, peritoneal blood levels increase, and symptoms progress to dyspnea or labored breathing, in addition to growing abdominal distension. Without treatment, blood loss can become acute, reuslting in hemorrhagic shock. The mortality rate for delayed hemoperitoneum is over 70 percent.

Diagnosis and Treatment
Doctors typically order an ultrasound, CT, and MRI to get the clearest picture of the fluid in the peritoneum. One of the safest ways to remove the fluid is paracentesis: the surgeon inserts a needle or catheter to draw out the blood, which they will then test for infection. In the case of a ruptured blood vessel, the surgeons use clamping and ligation to stop the bleeding or attempt to repair the damaged vessel.

Cauterization and Medications
Medications such as coagulants stop the bleeding and can give doctors time to evaluate options. In the case of a lacerated liver, for example, doctors may use argon plasma coagulation, an endoscopic cauterization technique that is a good option if issues prevent surgery. In the case of a ruptured spleen, the only recommendation is a splenectomy.

Scroll Down
for the Next Article
Popular Now on Facty Health
Disclaimer
This site offers information designed for educational purposes only. You should not rely on any information on this site as a substitute for professional medical advice, diagnosis, treatment, or as a substitute for, professional counseling care, advice, diagnosis, or treatment. If you have any concerns or questions about your health, you should always consult with a physician or other healthcare professional.